Every labour and birth is experienced differently. Labour pains may start with irregular small cramping feelings which build up to strong regular cramping pains felt not only in the abdomen but depending on factors such as the position of the baby, they can be felt in the back as well. These pains are caused by contractions of the muscles of the uterus and by pressure on the cervix – which opens gradually in response to these contractions.
The options for managing pain relief in labour can be discussed with the midwife (lead maternity carer) during pregnancy. As part of the labouring process women’s bodies release natural pain relief called endorphins – these are neurotransmitters that help reduce pain, reduce stress, and they are often referred to as “feel-good” hormones.
There are medication-based options, as well as non-medical options for pain relief. Preferences for pain management in labour can be included as part of a birth plan. It’s important to remember that women’s birth plan preferences can change when needed, and this includes choices previously made about pain relief during pregnancy. Midwives support women with their decisions and/or changes of plans. One to one, continuity of midwifery care supports women to manage their labours and increases maternal satisfaction with the birthing experience.
Non-medical options for pain relief
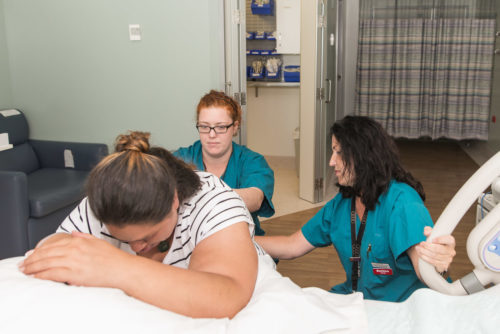
These include breathing techniques, back massage, acupuncture, acupressure, immersion in water, either in a bath or birthing pool, and a warm shower if immersion in water is not available. The position of the labouring woman is also important and can make a difference to both the woman’s experience and the progress of labour. Staying mobile during the first stage of labour, standing during contractions, being supported to stay upright, or using a birthing ball can support labour progress.
Key factors to support non-medical pain management during labour
- Support during labour and birth
- A known midwife providing continuity of care throughout pregnancy, labour, and birth
- Using water – a birthing pool
- Comfort measures – for example, massage, warm packs
- Staying mobile as much as possible /adjusting position during contractions